IMPORTANT QUESTIONS THAT ONE MUST ASK A NEUROLOGIST REGARDING STROKE
If you’ve been diagnosed with stroke, there are several key questions that you should ask your Neurologist like
- What is a stroke?
- What are the symptoms of a stroke?
- What is a mini-stroke or transient ischemic attack (TIA)?
- Does having a TIA increase my risk of a stroke?
- What are the risk factors for having a stroke?
- How is a stroke diagnosed?
- What are the treatment options for stroke?
- If I’ve had a stroke, do I have an increased risk for another stroke?
- When are blood thinners necessary? How is this decision determined?
- What are the differences between blood thinning medications? How do I know which one is right for me?
- What are the risks of blood thinning medications?
- How can strokes be prevented?
- How common are strokes?
- Are strokes hereditary?
Question 1. What exactly is a stroke?
Answer: Strokes, also known as cerebrovascular accidents (CVA), occur when blood flow in part of the brain is interrupted, denying brain tissue oxygen and nutrients. Damage to or death of brain cells can occur within minutes of such an event.
Question 2: Why Does a Stroke Happen and what are the types of strokes?
Answer: All strokes are caused by a lack of blood supply to the brain, leading to tissue injury, and resulting in the death of vital cells of the brain known as neurons.
There are two types of strokes, Ischemic and Haemorrhagic.
A. Ischemic stroke occurs when a blood vessel carrying blood to the brain is blocked by a blood clot. This causes a lack of blood to the brain. High blood pressure is the most important risk factor for this type of stroke. Ischemic strokes account for more than 80 percent of all strokes.
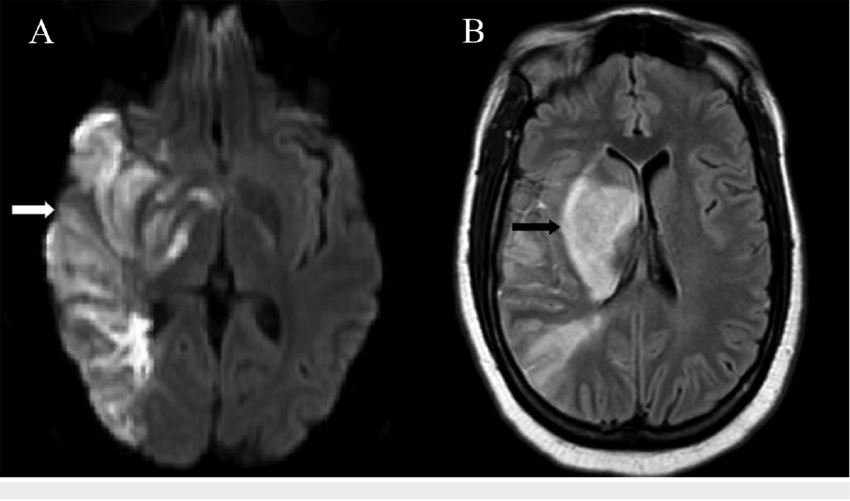
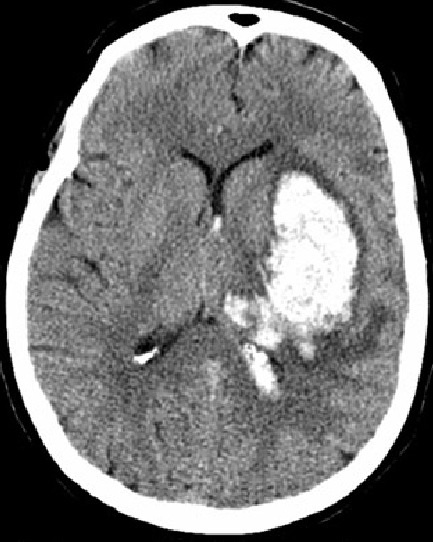
B. Haemorrhagic stroke is caused by bleeding in the brain, by either a ruptured brain aneurysm or a weakened bloodvessel leak.
Blood spills into or around the brain and creates swelling and pressure, damaging cells and tissue in the brain. They are less common. Only approximately 15 percent of all strokes are haemorrhagic, but they are responsible for about 40 percent of all stroke deaths.
Question 3: How do you identify a stroke?
Answer: The earlier you can recognize that you or a loved one are having a stroke, the better. It’s easy to identify a stroke by remembering the “F.A.S.T.” acronym.
F: Face drooping. During a stroke, one side of the face can become numb or droop. This can cause a person’s smile to appear uneven.
A: Arm/Leg weakness. A stroke will cause weakness in one arm or a feeling of numbness. If you ask a person who is having a stroke to raise both of their arms, one will drift downward.
S: Speech difficulty. Someone who is having a stroke will probably not be able to speak properly. Their words will be slurred, or it will be hard to understand them. They often will struggle to repeat a simple sentence.
T: Time to visit a Neurologist. If a friend or loved one is exhibiting any of these symptoms, call Neurologist and get to a hospital. Don’t hesitate! Even if only some of the symptoms are present, it’s better to be safe than sorry.
Be sure to take note of the time that the stroke symptoms started to show, even if they end up going away.
Question 4: How to diagnose a stroke and what investigations are required?
Answer: Clinical examination and brain imaging are necessary to diagnose a stroke. Brain imaging includes CT scan of head, MRI Brain, CT Angiography of head and neck vessels.
Question 5: Can stroke patients recover fully?
Answer: Yes, it is possible to recover completely from a stroke. Of all stroke patients, 10 percent will make a full recovery, while 25 percent will recover with minor impairments. Some patients (40 percent) will require special care due to more severe impairments, and 10 percent of individuals who had a stroke will need a nursing home or long-term care facility. Unfortunately, 15 percent of stroke patients die after their stroke.
- Strokes have a big impact on the brain and nervous system, and parts of the brain can experience cell damage.
- Fortunately, the damage is sometimes temporary, and even in cases where the stroke permanently kills brain cells, healthy areas of the brain have been known to take over for the damaged portions.
- This type of recovery varies from patient to patient and cannot be predicted, but even stroke patients with severe damage sometimes make unexpected recoveries.
- Rehabilitation and therapy can help the recovery process both physically and mentally.
Question 6: How long does it take to recover from a stroke?
Answer: Most stroke patients will need some form of rehabilitation, and the recovery timeline varies by the individual. Some stroke patients recover rather quickly, but if the stroke or the related complications were severe, it can take months or years.
The rehab process will change over time depending on the particular patient’s needs and progress.
Question 7: Can stress cause a stroke?
Answer: Yes, stress can absolutely be a contributing factor toward a stroke.
While minor day-to-day stress will probably not increase your chance of a stroke, chronic or long-term stress very well could.
A 2012 study published in the Journal of Neurology; Neurosurgery & Psychiatry found that individuals who reported chronic stress over the past year were four times more likely to have a stroke than those who did not have chronic stress in their lives.
Question 8: Why do stroke survivors have seizures after their stroke?
Answer: Just as physical wounds like cuts leave scars, a stroke can scar the brain. This impacts the electrical activity of the brain, sometimes leading to seizures.
Seizures are more common in stroke patients who had a hemorrhagic (bleeding) stroke, as opposed to an ischemic stroke.
Question 9: How can a caregiver keep a stroke survivor motivated?
Answer: Recovering from a stroke can feel daunting and overwhelming, and it can be hard for a stroke patient to find the motivation needed to recover. Stroke patients commonly suffer from apathy and depression.
If you are a friend, family member, or caregiver of a stroke patient, do your best to keep them motivated and thinking positively.
Question 10: Can young people have strokes?
Answer: Contrary to popular belief, a person of any age can suffer from a stroke. This includes teenagers, children, and even infants. Considering that people of all ages can have a stroke, it’s all the more important to know and recognize the warning signs.
Question 11: How do strokes affect speech?
Answer: One of the most common side effects of a stroke is trouble with speech. Because a stroke can damage the part of the brain that deals with language, many stroke patients are left with difficulty speaking or comprehending speech.
Question 12: Risk factors for stroke
Answer: Anyone can have a stroke at any age. But your chance of having a stroke increases if you have certain risk factors. Some risk factors for stroke can be changed or managed, while others can’t.
Risk factors that can be changed or medically managed:
- High blood pressure.
- Heart disease. Heart disease is the second most important risk factor for stroke, and the major cause of death among survivors of stroke.
- Diabetes. People with diabetes are at greater risk for a stroke than someone without diabetes.
- Smoking. Smoking almost doubles your risk for an ischemic stroke.
- Birth control pills (oral contraceptives)
- History of TIAs (transient ischemic attacks). TIAs are often called mini-strokes. They have the same symptoms as stroke, but the symptoms don’t last. If you have had one or more TIAs, you are almost 10 times more likely to have a stroke than someone of the same age and sex who has not had a TIA.
- High red blood cell count.
- High blood cholesterol and lipids.
- Lack of exercise
- Obesity
- Excessive alcohol use. More than 2 drinks per day raises your blood pressure. Binge drinking can lead to stroke.
- Illegal drugs. IV (intravenous) drug abuse like cocaine carries a high risk of stroke from blood clots (cerebral embolisms).
- Abnormal heart rhythm.
- Cardiac structural abnormalities. Damaged heart valves (valvular heart disease) can cause long-term (chronic) heart damage.
Risk factors for stroke that can’t be changed:
- Older age.
- Race. African Americans have a much higher risk for death and disability from a stroke than whites. This is partly because the African-American population has a greater incidence of high blood pressure.
- Gender. Stroke occurs more often in men, but more women than men die from stroke.
- History of prior stroke. You are at higher risk for having a second stroke after you have already had a stroke.
- Heredity or genetics. The chance of stroke is greater in people with a family history of stroke.
Question 13: What is the “golden hour?”
Answer: The golden hour is a concept in which very rapid therapy is more effective than later therapy.
Then Golden hour in stroke is 4.5 hours.
- The reason it is “golden” is that stroke patients have a much greater chance of surviving and avoiding long-term brain damage if they arrive at the hospital and receive treatment within Golden hour.
- Treatment within the golden hour is more successful because patients are candidates for the powerful clot-busting drug known as tPA (short for tissue plasminogen activator), which must be given within this Golden hour after a stroke.
- The golden hour reinforces the importance of reacting quickly to stroke symptoms because “time lost is brain lost.”
Question 14: What is the time frame to receive tPA (injection for dissolving clot) for an Ischemic stroke? Have the guidelines changed?
Answer: After a stroke, you’ve got very little time to get treatment. A drug called tissue plasminogen activator (tPA) dissolves clots and restores blood flow. The drug must be given as soon as possible after a stroke.
With every passing minute, more brain cells die.
Current guidelines recommend benefit of tPA for up to 4.5 hours after a stroke.
Question 15: Are There Any Things I Can Do to Lessen the Likelihood of Having Another Stroke?
Answer: There are many things that a stroke survivor can do to help lower their risk of another stroke. They include the following tips:
- Know Your Numbers – Blood Pressure, Blood Sugar, and Cholesterol
- Medication Compliance
If you feel you are having side effects related to medication, contact your doctor right away for options, and do not stop taking medication.
It can be very common for a stroke survivor to stop taking medications if they feel as if it is causing side effects but please do not stop taking them without talking to your team as stopping the use of medications can cause other serious health concerns, especially following a stroke.
- Getting a Healthy Amount of Activity
Researches support the need for aerobic activity to support after having a stroke. Even if the stroke survivor is unable to ambulate following a stroke, completing wheelchair-based activities such as arm yoga or riding an arm bike use can increase blood flow throughout the body.
Talk to your physical and occupational therapist for safe activity progression and guidance.
- Eating a Balanced and Healthy Diet
Diets with a high percentage of fruits and vegetables have been shown to help lower cholesterol, which can be a stroke risk factor.
- Stop Smoking
If you smoke, stop. Smoking has been proven time and time again to cause serious health conditions such as heart and vascular conditions which can both lead to stroke.